Lymphovenous Anastomosis: A Promising Surgical Approach for Alzheimer’s Disease
Emerging research indicates that a minimally invasive technique known as lymphovenous anastomosis (LVA), occasionally referred to as lymphovenous bypass, holds considerable promise as a therapeutic intervention for Alzheimer’s disease (AD). This innovative procedure is highlighted in a dedicated article featured in the March edition of Plastic and Reconstructive Surgery, a respected publication in the field.
Dr. Chew Khong Yik, the principal author and a Senior Consultant in the Department of Plastic, Reconstructive & Aesthetic Surgery at Singapore General Hospital (SGH), explains, “LVA introduces a groundbreaking surgical method aimed at correcting lymphatic dysfunction in the brain, which could be a critical element in both the onset and advancement of Alzheimer’s disease.” He emphasizes, however, that extensive additional investigations are essential to substantiate the procedure’s genuine advantages. The research effort was spearheaded by SGH in collaboration with experts from Duke-NUS Medical School and the National Neuroscience Institute, all located in Singapore.
Enhancing Toxin Clearance Through Lymphovenous Anastomosis in Alzheimer’s Patients
Lymphovenous anastomosis, or LVA, involves a straightforward yet precise surgical process where delicate lymphatic vessels are meticulously joined with adjacent blood vessels to optimize lymphatic circulation. This methodology is well-established in medical practice, particularly for alleviating lymphedema—a debilitating condition characterized by severe swelling due to impeded lymph flow, frequently arising as a side effect of cancer therapies.
Over the past several years, accumulating scientific evidence has pointed to the role of compromised lymphatic drainage within the brain, termed glymphatic flow due to its dependence on glial cells, in fostering pathological changes associated with Alzheimer’s disease. These changes encompass the buildup of amyloid-beta plaques and tau protein aggregates. Disruptions in glymphatic flow are believed to hinder the efficient removal of harmful neurotoxins, with this clearance process being especially active during periods of sleep. While various lifestyle modifications and pharmacological interventions have been proposed to bolster cerebral lymphatic function, their impact has generally proven modest at best.
LVA works by forging a direct linkage between lymphatic channels and venous structures, effectively circumventing any obstructions or impairments in the natural lymphatic routes. This results in a sustained, passive enhancement of glymphatic activity. Specialists in plastic and reconstructive surgery possess the requisite microsurgical expertise and in-depth knowledge of head and neck anatomy, positioning them uniquely to execute this procedure effectively.
Preliminary clinical investigations have demonstrated encouraging outcomes from LVA in individuals diagnosed with Alzheimer’s disease. Participants have exhibited notable improvements in standardized cognitive assessments, alongside remarkable enhancements in both mental acuity and physical capabilities in certain instances. Furthermore, some research has correlated these observable clinical advancements with objective measures of augmented lymphatic circulation.
Dr. Chew notes, “The collective findings from these initial studies affirm the procedure’s safety profile and its potential to yield cognitive improvements in Alzheimer’s patients, thereby justifying the need for more rigorous validation through larger-scale trials.” To robustly demonstrate LVA’s efficacy specifically for Alzheimer’s, the researchers propose several key methodological considerations, outlined as follows:
- Precise patient selection protocols, focusing on those with verified mild to moderate Alzheimer’s disease diagnoses.
- Consistent surgical methodologies, incorporating comprehensive preoperative evaluations to identify optimal lymphatic and vascular targets.
- Structured protocols for tracking and assessing variations in cognitive performance over time.
- Empirical validation of the biological pathways through which glymphatic restoration translates into tangible clinical benefits.
- Comprehensive documentation of procedural risks, possible adverse events, and complication rates associated with LVA.
In their concluding remarks, Dr. Chew and his colleagues assert, “LVA offers an innovative therapeutic pathway that could synergize with conventional Alzheimer’s treatments, instilling fresh optimism in tackling the underlying disease mechanisms.” They advocate for multifaceted, extended-duration clinical trials to explore LVA’s role not merely as a supplementary option but potentially as a viable primary intervention for Alzheimer’s and possibly other neurodegenerative conditions as well.
Understanding the Science Behind Glymphatic Flow and Alzheimer’s Pathology
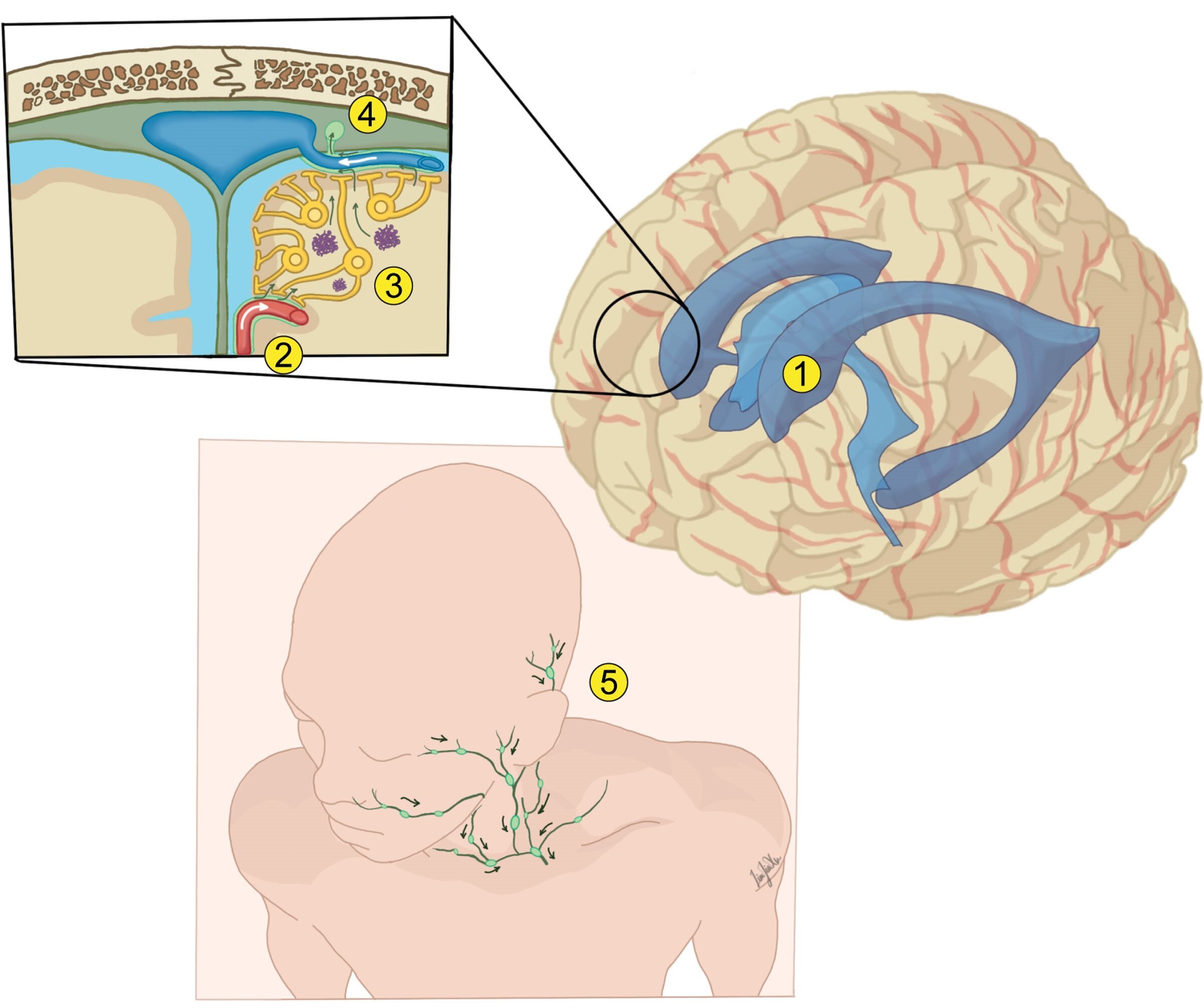
The glymphatic system represents a relatively recently discovered network responsible for maintaining the brain’s internal environment by facilitating the removal of metabolic waste products. In healthy individuals, this system operates most efficiently during sleep, when cerebrospinal fluid flows through perivascular spaces to flush out toxins like amyloid-beta, a protein fragment strongly implicated in Alzheimer’s neurodegeneration. When glymphatic function falters—often due to aging, vascular issues, or inflammation—waste accumulates, promoting plaque formation and neuronal damage that characterize AD progression.
Meningeal lymphatics, superficial vessels draining the brain’s outer coverings, complement this system by channeling cleared materials into cervical lymph nodes for immune processing. Impairments here exacerbate AD pathology. LVA’s appeal lies in its capacity to restore these pathways surgically, potentially offering a more direct and reliable enhancement than pharmacological or behavioral strategies alone.
Clinical Evidence and Future Research Directions
Early case series and small cohort studies have reported not only cognitive stabilization or gains but also improvements in daily functioning and biomarkers indicative of better waste clearance. For example, imaging modalities like near-infrared fluorescence lymphography have visualized enhanced flow post-LVA, correlating with patient-reported benefits. These findings, while preliminary, challenge the dominance of purely pharmacological paradigms in AD management and spotlight surgical innovation.
To advance this frontier, future protocols must prioritize randomized controlled trials comparing LVA against sham procedures or standard care. Long-term follow-up will be crucial to assess durability of effects, especially given AD’s relentless course. Multidisciplinary teams—including neurologists, neurosurgeons, and lymphologists—will be vital for refining techniques, such as optimal anastomosis sites in the neck to maximize cranial drainage.
Safety data thus far is reassuring, with minimal complications akin to those in lymphedema applications: transient swelling, minor infections, or rare vessel thrombosis. However, AD patients’ comorbidities necessitate tailored risk stratification.
Broader Implications for Neurodegenerative Disorders
Beyond Alzheimer’s, LVA’s principles could extend to conditions sharing glymphatic impairments, such as Parkinson’s disease, where alpha-synuclein aggregates mirror amyloid pathology, or traumatic brain injury sequelae. This surgical paradigm shift underscores the value of addressing clearance deficits directly, potentially reshaping treatment landscapes for proteinopathies.
Publication details: Yu-Hsin Yen et al., Exploring Lymphovenous Anastomosis for Alzheimer Disease: Addressing Brain Lymphatic Dysfunction, Feasibility, and Outcome Metrics, Plastic & Reconstructive Surgery (2025). DOI: 10.1097/prs.0000000000012364