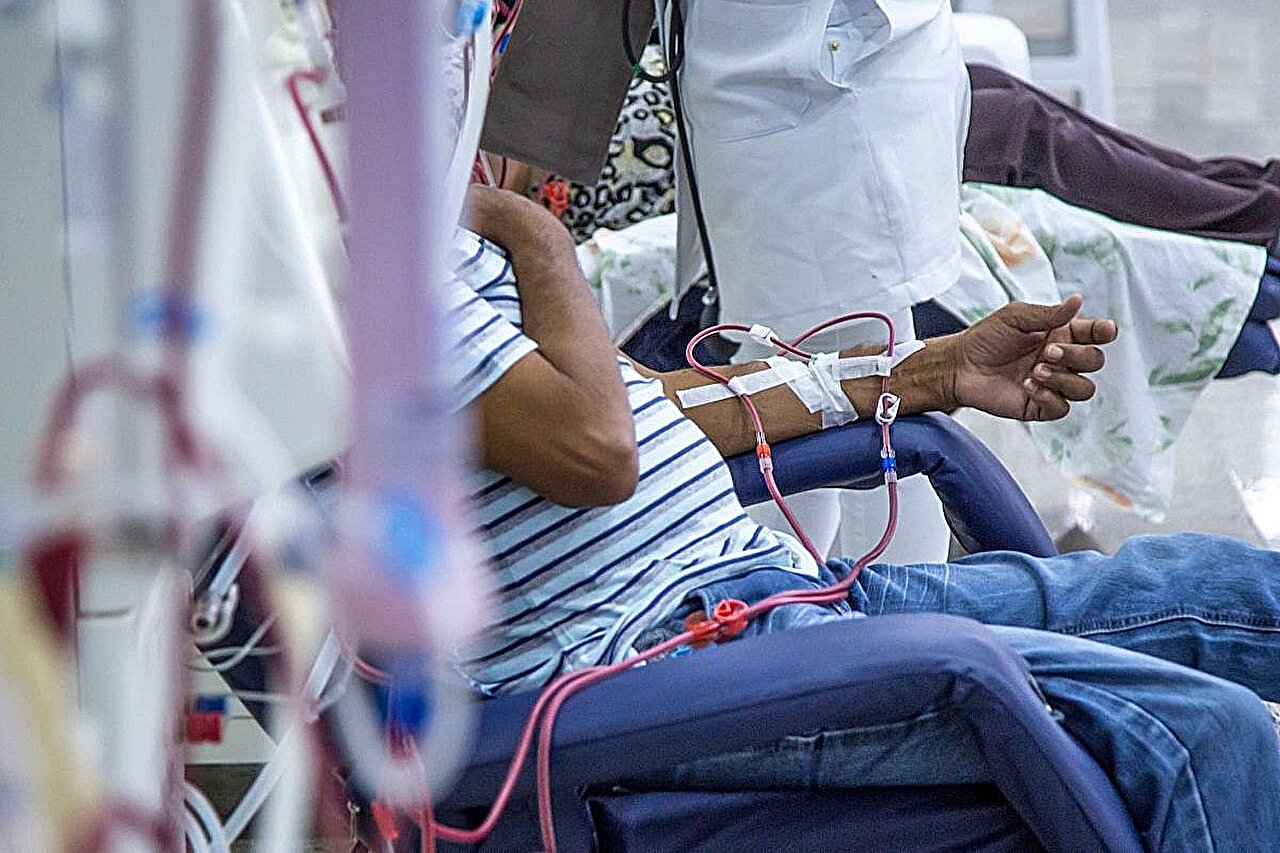
Engaging with primary care services proves beneficial for individuals undergoing hemodialysis, as it correlates with significantly decreased mortality rates, according to recent research disseminated online in the esteemed journal Kidney Medicine.
Dustin Le, M.D., affiliated with Thomas Jefferson University located in Philadelphia, along with his team of researchers, meticulously examined the relationship between primary care utilization over the preceding year and various clinical outcomes. Their comprehensive analysis encompassed a substantial group of 122,496 Medicare beneficiaries who were actively receiving hemodialysis treatments.
The investigation revealed that a notable 60 percent of participants within this extensive cohort had accessed primary care services on at least one occasion during the year prior to the study period. This engagement with primary care providers demonstrated a compelling link to reduced instances of all-cause mortality, registering a hazard ratio (HR) of 0.90. Furthermore, the data indicated lower cardiovascular mortality with an HR of 0.96, and a particularly pronounced decrease in mortality due to infections, evidenced by an HR of 0.81.
Beyond these mortality benefits, the study also identified associations with heightened healthcare utilization patterns. Specifically, primary care use was connected to elevated rates of initial hospitalizations, with an HR of 1.04. Similarly, there was an uptick in the first visits to emergency departments or urgent care facilities, reflected by an HR of 1.06. Additionally, subsequent engagements with primary care services showed a dramatically higher likelihood, quantified by an impressive HR of 4.30.
In summarizing their findings, the research team emphasized, “In conclusion, among U.S. Medicare beneficiaries already on in-center hemodialysis, receipt of at least one primary care visit in the previous year was associated with lower all-cause mortality and a small increase in health care utilization.” This statement underscores the dual impact of primary care involvement, balancing mortality reduction against modest rises in service usage.
The authors further advocate for expanded investigations into the precise role and underlying mechanisms through which primary care influences outcomes for patients dependent on hemodialysis. Such deeper exploration could yield valuable insights with broad implications for population health management strategies tailored to individuals grappling with kidney failure necessitating hemodialysis therapy.
This study highlights the critical importance of integrating primary care into the ongoing management of hemodialysis patients. For those enduring the rigors of dialysis, regular interaction with primary care physicians may offer a protective shield against premature death, particularly from cardiovascular events and infections, which remain leading causes of mortality in this vulnerable population.
Hemodialysis itself is a life-sustaining procedure for patients whose kidneys have failed to an extent that they can no longer adequately filter waste products from the blood. Typically performed in specialized centers three times per week, each session lasting several hours, it demands significant commitment from patients. Amid this intensive regimen, the addition of primary care oversight appears to enhance overall survival prospects without exorbitantly inflating healthcare costs through excessive utilization.
The modest increase in hospitalizations and emergency visits noted in the study may reflect proactive care that catches issues early, potentially preventing more severe complications down the line. Primary care providers are uniquely positioned to coordinate multidisciplinary care, monitor chronic conditions, and promote preventive measures that dialysis-centric care alone might overlook.
Policymakers and healthcare administrators should take note of these results, as they suggest that incentivizing primary care engagement among dialysis patients could lead to substantial public health gains. Medicare programs, in particular, might benefit from targeted initiatives to bridge gaps in primary care access for this group, ultimately fostering better long-term outcomes and resource efficiency.
For clinicians, the findings reinforce the value of maintaining close ties with primary care even for patients entrenched in nephrology follow-up. Simple encouragement to schedule annual or more frequent primary care appointments could translate into tangible survival advantages, empowering patients with a more holistic approach to their health.
Future studies might delve into qualitative aspects, such as patient experiences with primary care integration, barriers to access, and optimal visit frequency. Randomized controlled trials could further validate these observational associations, providing higher levels of evidence to guide clinical guidelines and reimbursement policies.
In essence, this research illuminates a straightforward yet powerful intervention—leveraging primary care—that holds promise for improving the quality and length of life for hemodialysis patients, a group often facing elevated mortality risks due to the complexities of end-stage renal disease.