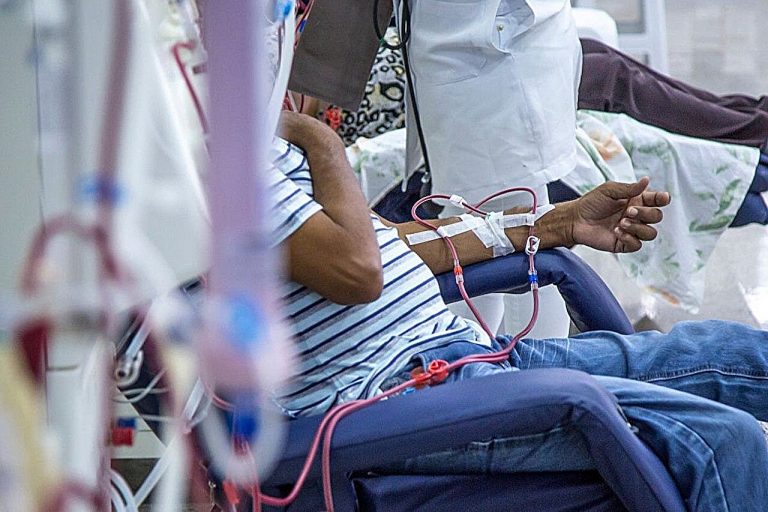
Investigators from Mass General Brigham spearheaded a comprehensive national study revealing that socioeconomic challenges such as financial difficulties, food insecurity, limited access to healthcare, and various other social determinants are strongly associated with elevated risks of developing long COVID.
Long COVID is characterized by a broad spectrum of symptoms that either emerge or continue for at least three months following an infection with the SARS-CoV-2 virus. Over recent years, scientists have made substantial progress in understanding the prevalence, manifestations, and impacts of long COVID thanks to the ongoing longitudinal Researching COVID to Enhance Recovery (RECOVER) Initiative. However, the influence of social risk factors on the likelihood of developing long COVID has not been fully explored until now. In a fresh examination of data from the RECOVER-Adult cohort, researchers at Mass General Brigham identified that individuals facing social risk factors experience two to three times the risk of long COVID. These factors encompass financial hardship, food insecurity, encounters with medical discrimination, and forgoing necessary medical care due to expenses. The results of this analysis appear in the journal Annals of Internal Medicine.
Understanding the Impact of Social Risks During and Beyond the Pandemic
“Throughout the COVID-19 pandemic, it became evident how pivotal social risk factors were in shaping who contracted the virus, the intensity of their illness, and the associated mortality rates,” explained lead author Candace Feldman, MD, MPH, ScD, from the Division of Rheumatology, Inflammation and Immunity at Brigham and Women’s Hospital (BWH), which is a key component of the Mass General Brigham healthcare network. “Our goal with this research was to investigate if these same social elements continue to exert a profound influence on the persistent, chronic symptoms that linger for months or even years post-SARS-CoV-2 infection.”
For this investigation, the research team evaluated data from 3,700 participants in the RECOVER-Adult cohort. All participants had contracted SARS-CoV-2 during the period dominated by the Omicron variant, filled out an initial survey capturing their social and economic circumstances at the time of infection, and subsequently completed a follow-up survey at the six-month mark to report on long COVID symptoms. These individuals hailed from 33 states across the U.S., as well as Washington, D.C., and Puerto Rico, with enrollment occurring from October 2021 through November 2023.
Detailed Assessment of Social Risk Factors
During the baseline survey, the scientists measured four primary categories of individual-level social risk factors. These included economic instability, barriers related to education and language access, obstacles in healthcare access and quality, and deficiencies in social and community support. To gather this information, they employed targeted questions alongside established, validated survey instruments. Additionally, the team incorporated ZIP code-based data to evaluate community-level risks, such as household crowding.
The analysis accounted for confounding variables like hospitalization due to SARS-CoV-2 (serving as an indicator of infection severity), prior vaccination status, pregnancy, age, sex, race, and ethnicity. Even after these adjustments, the study uncovered robust links between almost every individual-level social risk factor examined and a heightened probability of long COVID. Moreover, the accumulation of multiple social risk factors correlated with progressively greater risks. Residence in neighborhoods characterized by higher household crowding also emerged as a significant predictor of increased long COVID risk.
Disparities and Equity Considerations
The study highlighted a notably heavier load of social risk factors among racially and ethnically minoritized populations. That said, the effects of these social risks on long COVID development appeared consistent across white, Black, and Hispanic groups, without substantial differences in impact.
Looking ahead, researchers involved in the RECOVER Initiative aim to explore whether these patterns hold true for pediatric cases of long COVID. They are also interested in pinpointing if particular long COVID symptoms align with specific social risk factors. Furthermore, the team plans to delve into symptoms persisting for a full year or more, aiming to clarify the role social determinants play in their endurance.
Implications for Future Interventions and Chronic Disease Management
“Even as COVID-19 infection rates have declined, long COVID remains a debilitating chronic condition affecting numerous individuals,” noted senior author Elizabeth Karlson, MD, MS, also from the Division of Rheumatology, Inflammation and Immunity at BWH. “Similar to many other chronic illnesses, a person’s social surroundings—encompassing economic, community, and healthcare elements—profoundly shape their vulnerability to long COVID. To mitigate poor outcomes effectively, especially for those burdened by multiple social risks, upcoming interventions will need to tackle these underlying issues head-on.”
Research Team and Contributors
In addition to lead authors Feldman and Karlson, the Mass General Brigham contributors included Leah Santacroce, Ingrid V. Bassett, Tanayott Thaweethai, Yuri Quintana, Bruce D. Levy, and Cheryl R. Clark.
The broader authorship roster features Radica Alicic, Rachel Atchley-Challenner, Alicia Chung, Mark P. Goldberg, Carol R. Horowitz, Karen B. Jacobson, J. Daniel Kelly, Stacey Knight, Karen Lutrick, Praveen Mudumbi, Sairam Parthasarathy, Heather Prendergast, Nasser Sharareh, Judd Shellito, Zaki A. Sherif, Brittany D. Taylor, Emily Taylor, Joel Tsevat, Zanthia Wiley, Natasha J. Williams, Lynn Yee, Lisa Aponte-Soto, Jhony Baissary, Jasmine Berry, Alexander W. Charney, Maged M. Costantine, Alexandria M. Duven, Nathaniel Erdmann, Kacey C. Ernst, Elen M. Feuerriegel, Valerie J. Flaherman, Minjoung Go, Kellie Hawkins, Vanessa Jacoby, Janice John, Sara Kelly, Elijah Kindred, Adeyinka Laiyemo, Emily B. Levitan, Jennifer K. Logue, Jai G. Marathe, Jeffrey N. Martin, Grace A. McComsey, Torri D. Metz, Tony Minor, Aoyjai P. Montgomery, Janet M. Mullington, Igho Ofotukun, Megumi J. Okumura, Michael J. Peluso, Kristen Pogreba-Brown, Hengameh Raissy, Johana M. Rosas, and Upinder Singh, along with Timothy VanWagoner.
Disclosures and Funding Sources
Feldman discloses receiving grant funding to her institution for health equity studies and provides consulting services to various organizations on topics unrelated to this work. Knight reports research funding from Janssen. Other authors including Alicic, Parthasarathy, Aponte-Soto, Singh, Levitan, and Mullington acknowledge NIH or alternative research grants and consulting fees not connected to this publication.
This research received partial funding from the National Institutes of Health through grants OTA OT2HL161841, OTA OT2HL161847, and OTA OT2HL156812.